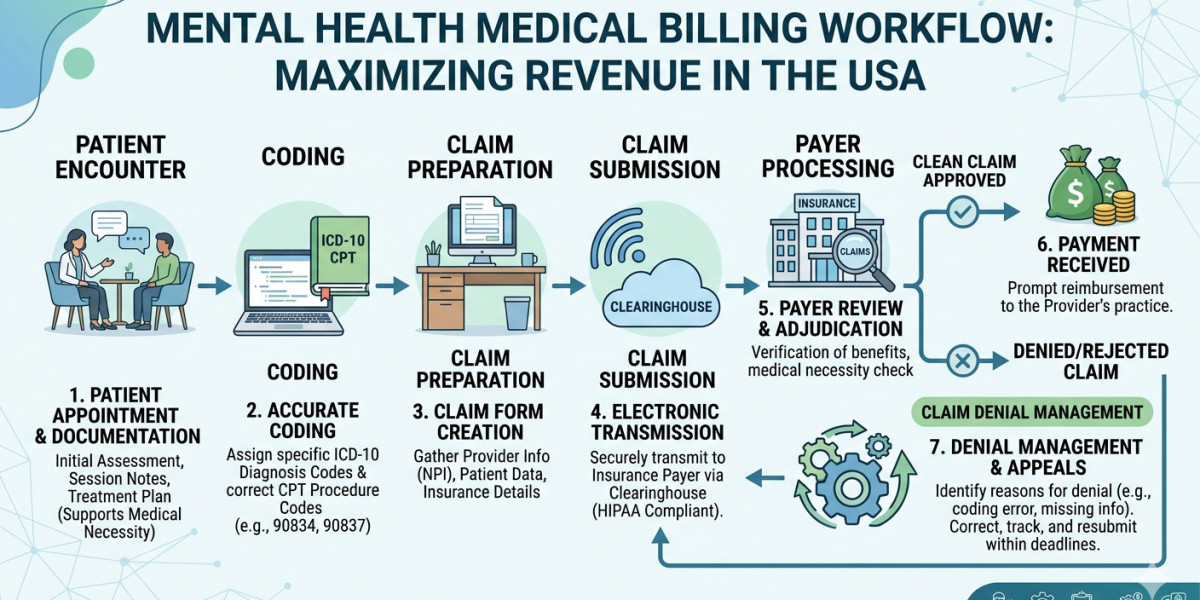
Mental health practices across the United States are growing rapidly, but so are the complexities of billing. From insurance policies to coding accuracy and compliance requirements, providers often struggle to maintain steady cash flow while delivering quality care. This is where a clear understanding of medical billing for mental health becomes essential.
Whether you run a private therapy practice, a behavioral health clinic, or a multi-specialty facility, optimizing your billing process can significantly improve your revenue cycle and reduce administrative stress.
Introduction: Why Mental Health Billing Matters
Mental health billing is different from general medical billing due to:
- Frequent use of time-based CPT codes
- Strict payer guidelines for psychotherapy services
- Complex documentation requirements
- High denial rates due to coding errors
- Variations in insurance coverage for behavioral health
A well-structured mental health billing system ensures faster reimbursements, fewer denials, and better financial stability.
What is Medical Billing for Mental Health?
Medical billing for mental health refers to the process of submitting and managing insurance claims for services like psychotherapy, psychiatric evaluations, counseling, and medication management.
It involves:
- Patient eligibility verification
- Accurate coding using CPT and ICD codes
- Claim submission to insurance payers
- Payment posting and reconciliation
- Denial management and appeals
Unlike traditional healthcare billing, mental health billing requires a deep understanding of therapy session durations, modifiers, and payer-specific rules.
Key Components of Mental Health Billing
1. Patient Eligibility and Insurance Verification
Before any session, verifying insurance coverage is critical. Many claims get denied simply because the service isn’t covered under the patient’s plan.
2. Accurate Coding
Coding and billing for mental health services rely heavily on:
- CPT codes for therapy sessions (30, 45, 60 minutes)
- ICD-10 codes for diagnoses
- Modifiers for telehealth or extended sessions
Even a minor error can lead to claim rejection.
3. Documentation Compliance
Therapists must document:
- Session duration
- Treatment plan
- Progress notes
This supports claims during audits and ensures compliance.
4. Claim Submission and Follow-ups
Timely claim submission reduces delays. Regular follow-ups help track unpaid or denied claims.
5. Denial Management
Denials are common in mental health billing. Efficient appeal processes help recover lost revenue.
Common Challenges in Billing for Mental Health Therapists
Mental health providers face several billing-related challenges:
- Confusing payer policies
- Frequent claim denials
- Time-consuming administrative work
- Credentialing delays
- Difficulty in billing Medicare for mental health services
These challenges often force providers to spend less time on patient care and more on paperwork.
Why Outsourced Billing for Mental Health is Growing
Many practices now prefer outsourced billing for mental health to improve efficiency and reduce workload.
Benefits include:
- Reduced administrative burden
- Improved claim acceptance rates
- Faster reimbursements
- Access to billing experts
- Cost-effective operations
Choosing the best outsource mental health billing and coding services can significantly enhance your practice’s financial performance.
In-House vs Outsourced Mental Health Billing
In-House Billing
- Full control over operations
- Requires trained staff
- Higher operational costs
- Risk of errors if not specialized
Outsourced Billing
- Access to experienced professionals
- Lower overhead costs
- Better compliance and accuracy
- Scalable as your practice grows
Many providers also look for a cheap outsource mental health billing company, but it’s important to prioritize quality over cost.
Understanding Mental Health Billing and Credentialing Services
Credentialing is a crucial part of mental health billing. Without proper enrollment with insurance providers, claims cannot be processed.
Mental health billing and credentialing services help with:
- Provider enrollment
- Insurance panel approvals
- CAQH profile management
- Re-credentialing
Delays in credentialing can directly impact your revenue.
Best Practices for Efficient Mental Health Billing
To optimize your billing process, follow these proven strategies:
1. Use Accurate and Updated Codes
Regularly update CPT and ICD codes to avoid claim rejections.
2. Verify Insurance Before Every Visit
Even returning patients may have policy changes.
3. Maintain Clear Documentation
Detailed notes help in audits and appeals.
4. Automate Billing Processes
Use software tools for scheduling, billing, and reporting.
5. Monitor Key Performance Indicators
Track metrics like:
- Days in Accounts Receivable
- Claim denial rate
- First-pass acceptance rate
How Mental Health Medical Billing Impacts Revenue
A well-managed mental health medical billing system directly improves:
- Cash flow
- Operational efficiency
- Patient satisfaction
- Compliance with regulations
On the other hand, poor billing practices can lead to revenue leakage, delayed payments, and legal risks.
Choosing the Right Billing Services for Mental Health Clinics
When selecting billing services for mental health clinics, consider:
- Experience in behavioral health billing
- Knowledge of payer guidelines
- Transparent pricing
- Technology and reporting tools
- Dedicated account management
Reliable billing services for mental health ensure that your practice runs smoothly without financial disruptions.
The Role of Behavioral and Mental Health Billing Services
Behavioral and mental health billing services specialize in handling complex therapy billing requirements.
They provide:
- End-to-end revenue cycle management
- Accurate claim submission
- Denial tracking and resolution
- Compliance with HIPAA regulations
These services are especially beneficial for growing practices and multi-provider clinics.
Future Trends in Mental Health Billing
The mental health billing landscape is evolving with:
- Increased telehealth services
- AI-driven billing automation
- Value-based care models
- Integration of EHR and billing systems
Practices that adapt to these changes will have a competitive advantage.
How 247 Medical Billing Services Can Help
Partnering with a reliable billing company can transform your revenue cycle. 247 Medical Billing Services supports healthcare providers with:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
Their expertise ensures accurate claims, faster reimbursements, and reduced administrative stress, making them a trusted partner for mental health practices across the USA.
Conclusion
Medical billing for mental health is more than just submitting claims. It’s a critical component of your practice’s success. From accurate coding to efficient denial management, every step plays a role in maximizing revenue.
As the demand for mental health services continues to rise, adopting efficient billing practices or partnering with experienced professionals can help you stay ahead. Whether you choose in-house management or outsourced billing for mental health, the goal remains the same: streamline operations and focus on patient care.
FAQs
What is the difference between mental health billing and general medical billing?
Mental health billing focuses on time-based therapy sessions, strict documentation, and specialized coding, making it more complex than general medical billing.
Why are mental health claims often denied?
Common reasons include incorrect coding, missing documentation, and lack of insurance coverage verification.
Is outsourcing mental health billing cost-effective?
Yes, outsourced billing for mental health reduces administrative costs and improves claim accuracy, leading to better revenue.
What are the key codes used in mental health billing?
CPT codes for therapy sessions and ICD-10 codes for diagnoses are commonly used in mental health billing.
How long does it take to get credentialed with insurance providers?
Credentialing can take anywhere from 60 to 120 days, depending on the payer and documentation.
Can small practices benefit from mental health billing services?
Absolutely. Even small practices can improve efficiency and revenue by using professional mental health billing services.
What should I look for in a billing company?
Look for experience, transparency, compliance knowledge, and strong reporting capabilities when choosing billing services for mental health clinics.